Many people with cystic fibrosis will reach a time when they need a lung transplant. The success rate of transplants for people with CF is encouraging and recipients often enjoy a much better quality of life.
Lung transplantation may be an option for people with advanced lung disease caused by CF. Your CF specialist will decide if you can be assessed for transplantation.
A lung transplant requires a lot of planning and your CF team may begin to start discussing the possibility of a lung transplant before you actually require a transplant.
Numerous tests are carried out to ensure that the patient is suitable for receiving a transplant. The assessment process includes extensive clinical, physical and laboratory testing carried out by the transplant team, ensuring suitability for transplant. The process is generally spread over a week and patients have a support person with them during this time. The assessment for suitability for transplant also focuses on a patient’s psycho-social wellbeing, and includes identifying their support systems and plans/goals they have for the future.
Do not underestimate the importance of the psychosocial assessment part of the lung transplant assessment. Some of the issues raised include:

Financial planning is also vital. Many CF families will be saving money to cover the costs of having to be off work for months. Not only will the person having a transplant be off work, but their support person is often their partner, who will also have to take several weeks off work during the recovery process. Therefore, many people start making financial plans for this in the years leading up to a transplant.
Find out what financial help is availableAfter a person has been assessed for a transplant they are placed in four categories:
Active List – they are approved for transplant and will be considered for any donated organ that matches their blood group and body size.
Inactive List – they are approved for a transplant once their health deteriorates – these individuals are closely monitored for when it’s time to go on the active list.
Deferred – they may be a suitable candidate but may need to make lifestyle changes such as gaining or losing weight.
Declined - the transplant team has decided this person is unable to have a transplant. This could be related to compliance with on-going treatment, they may be too unwell for the operation, or other health-related reasons.
Some people are unable to have a lung transplant because they are a current smoker or because of other pre-existing health conditions including:
There is no way to know how long a person will be on the waiting list. The timing depends on medical need and also on the availability of a donor lung that is a good match. There is also a possibility that someone’s health can improve during this time and could be removed from the active list.
False alarms are also a possibility while on the active list. You could be called into hospital but arrive to find the lungs have deteriorated and no longer considered viable or other circumstances mean the transplant cannot go ahead. This can be very distressing but it is an unfortunate reality during the transplant process.
During the surgery an incision is made from under the patient's armpit, around to the sternum, and then back towards the other armpit; this is known as a clamshell incision. The least effective lung is removed first then the new lung is then placed and the blood vessels reattached. Then the second lung is transplanted.
After the operation patients are transferred to the intensive care ward for up to five days before being transferred to the Respiratory Ward and then later discharged to Hearty Towers in Green Lane where they will live with their support person in the same room while they get used to their medicine, treatment and learn how to maintain their health.
Visitors are initially limited at ICU to two family members at a time and everyone who enters the room should wash their hands thoroughly and practice good hygiene. It’s extremely important that visitors who are unwell do not visit until they have fully recovered.
Organ rejection can occur at any time but is more common in the first three months.
To prevent the body from rejecting the new lungs, individuals need to commit to taking immunosuppressive medication for the rest of their lives. Immunosuppressants assist the body to accept the new organ by lowering the body’s immune system.
In turn, however, this can result in individuals being susceptible to bacteria and infection (due to lowered immunity). Therefore, it is essential that individuals are vigilant with good hygiene practices for the ongoing maintenance of health and wellbeing.
Taking care of your new lungs is extremely important. Your transplant team will help you learn how to reduce the risk of infection and rejection, and to care for your lungs.
Good hygiene practices include:
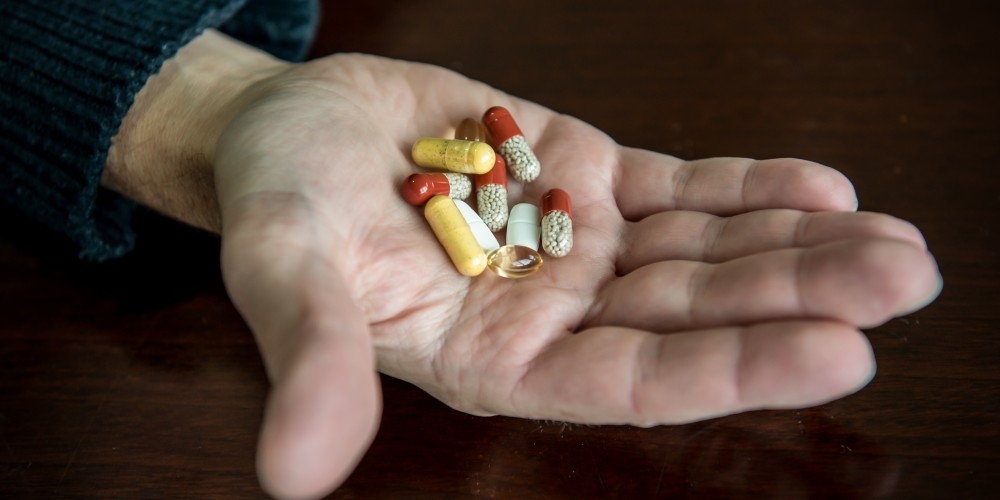
After the transplant, the new lungs do not have and will not develop CF, but the patient’s body still has CF in all other aspects such as sweat glands, pancreas, sinuses and reproductive organs. People will still need to take their usual medications for nutrition.
Research suggests that people with cystic fibrosis have better outcomes following transplant surgery because they have been used to taking medication and being cautious about infection risks their whole lives.
Once you’ve had your transplant your relationship with your CF team will change. Your new lungs no longer have cystic fibrosis, however, other organs are still affected by CF and ongoing medical care will still be necessary – some of which can be managed by your GP.
CFNZ provides significant support for people going through the lung transplant process. You can talk to your Field Worker about this support or browse financial assistance available.
CFNZ provides significant support for people going through the lung transplant process, including lung transplant assistance. You can talk to your Fieldworker about this support.
Once you’ve had your transplant your relationship with your CF team will change. Your new lungs no longer have cystic fibrosis, however, other organs are still affected by CF and ongoing medical care will still be necessary – some of which can be managed by your GP.